How to manage esophageal varices?
According to Best Gastroenterologist in Lahoreesophageal varices are enlarged vessels in the esophagus, that can break open and bleed. Read on to know more about esophageal varices and how to manage them:
What are esophageal varices?
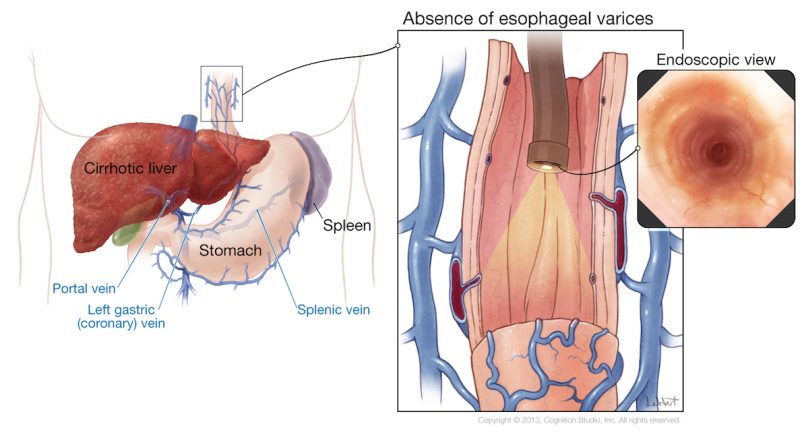
Esophageal varices are swollen vessels in the esophagus, which occur most commonly due to chronic liver disease and portal hypertension. If the blood flow to the liver is blocked by scarring as seen in liver cirrhosis, or blood clots, collateral blood vessels form around the esophagus and umbilicus. These blood vessels are fragile and cannot carry large volumes of blood; therefore, they are at the risk of rupturing and causing life-threatening bleeding.
What are the symptoms of esophageal varices?
The symptoms of esophageal varices are:
- Blood in vomitus
- Nausea and vomiting
- Light headedness and pallor if bleeding is chronic
- Black and tarry stools
- Loss of consciousness
Additional signs of liver disease include:
- Jaundice and yellowish discoloration of skin
- Abdominal ascites due to fluid buildup
- Easy bruising
- Itching on the skin
What are the causes of esophageal varices?
The causes of esophageal varices are:
- Chronic liver disease (CLD): chronic hepatitis, fatty liver disease, alcoholic liver disease and biliary disorders can result in scarring or cirrhosis of liver which can result in portal hypertension and formation of esophageal varices.
- Thrombosis or blood clot formation: any blood clot in the portal vein of the liver can result in portal hypertension and therefore varices formation.
- Microbial infection: parasitic infections like schistosomiasis can damage the liver, lungs and other organs, thereby resulting in portal hypertension and esophageal varices formation.
Who is at risk of developing bleeding esophageal varices?
Individuals who are at of bleeding of esophageal varices include:
- Large varices: if the varices are numerous and enlarged, the risk of bleeding is higher.
- Severe cirrhosis: with increasedscarring of liver or advanced cirrhosis, there are more varices in the esophagus, with increased risk of bleeding.
- Liver failure: with advanced liver disease and liver failure, the chances of bleeding esophageal varices rise.
- Alcohol use: continued alcohol use worsens the condition of the liver and increases variceal formation.
- High pressure in portal vein: with portal hypertension the odds of bleeding,rise.
What are the management options?
For esophageal varices, the primary aim is to decrease the chances of bleeding and decreasing the bleeding if it does occur. The treatment options therefore, include:
- Medication: beta blockerscan reduce blood pressure in the portal vein and decrease the chances of bleeding. Other drugs like octreotide and vasopressin can slow the blood flow in the portal veinand can be used after a bleeding episode.
- Elastic bands: with endoscopy, an elastic band can be applied around the bleeding varices to stop it.
- Restoring blood volume: blood can be transfused to replace the lost volume.
- TIPS: trans-jugular intrahepatic portosystemic shunt can directly carry blood from the liver to the heart, thereby decreasing varices formation. It is used when other treatments have failed.
- Liver transplant:is done for severe liver disease.
How can esophageal varices be prevented?
In chronic liver disease, there is little one can do to prevent esophageal varices from forming. However, there are steps one can take to prevent worsening of liver disease, which include:
- Alcohol: the liver is responsible for processing toxins alcohol out of the body; excessive drinking, therefore, is bad for the health of the liver. People with liver disease can stress it further with drinking. Giving up alcohol is, thus, better for people with liver disease.
- Healthy diet: plant-based diet with more fruits and vegetables is better for the body and the health of the liver.
- Exercising: maintaining a healthy weight and losing fat helps to reduce liver damage. High body fat and obesity predispose to liver disease, which is why losing weight can help prevent the complications of liver disease.
- Reducing risk of hepatitis: chronic liver disease (CLD) as induced by hepatitis B and C can increase the chances of developing portal hypertension and esophageal varices.Protecting oneself from hepatitis by getting vaccinated fromDr. Asad Sadiqand getting tested periodically for these viruses can help to reduce the risk of CLD and esophageal varices.